As the United States looks for ways to address the nation's opioid epidemic, acupuncturists in California see an opportunity to push their traditional Chinese healing technique into US mainstream medicine.
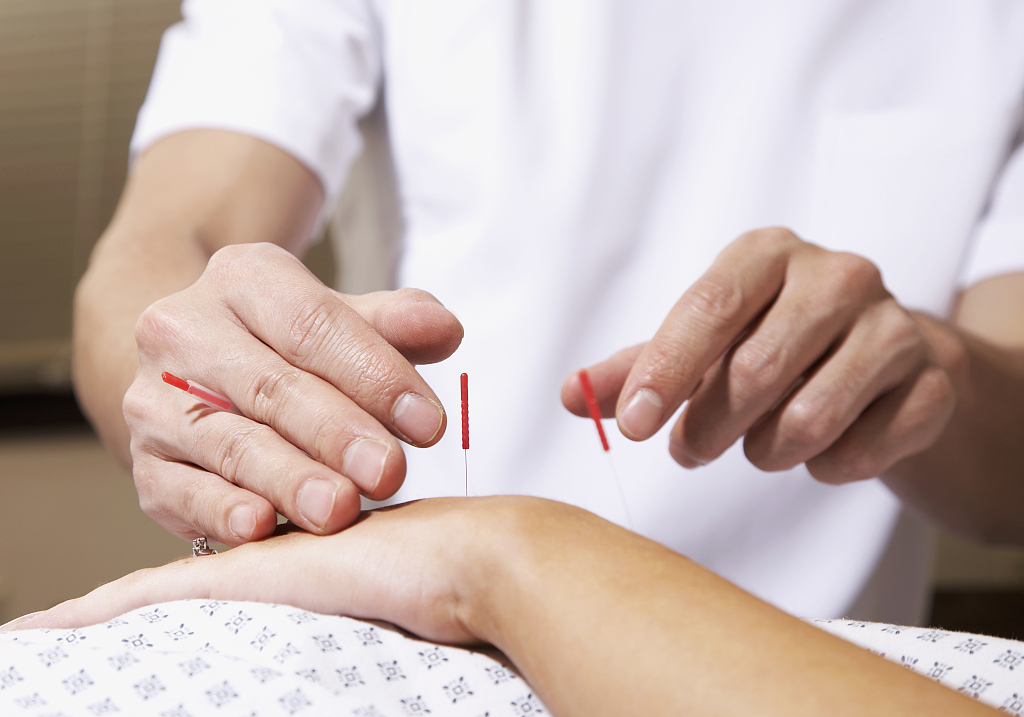
(File photo: VCG)
"It opens a door for us," said Sam Huang, a San Francisco-based acupuncturist and activist. "Acupuncture has never been recognized by the US mainstream like now."
A US House bill, HR 6, which became law in October, promotes opioid recovery and treatment. The law orders research into barriers to accessing nondrug alternatives to opioids within the Medicare program, a national health insurance program. It mentions acupuncture as one of the alternatives.
"It represents the first time in US history that acupuncture has been incorporated into a federal document," said Huang. "It will push acupuncture into the federal insurance program and eventually the US mainstream."
Each year, an estimated 42,249 individuals die from overdosing on opioids in the US, according to the Joint Commission, the largest healthcare accreditation body in the US.
The organization includes acupuncture as an evidence-based, nonopioid treatment option for pain in its advisory for health providers issued in August.
Practiced in China for thousands of years, acupuncture is one of the key components of traditional Chinese medicine to prevent or treat health problems.
California became the first state in the US to regulate acupuncture in 1975. Now, 47 of the 50 states have similar regulations.
The country has about 38,000 licensed acupuncturists, and one-third of them are of Chinese descent, according to the American Association of Chinese Medicine and Acupuncture, a San Francisco-based advocacy group. California has 18,000 licensed acupuncturists.
Though acupuncture has gained increasing popularity in the US in the past 40 years, its scope of practice in the US is still limited, and most insurance programs don't cover it, said Jun Hu, president of the association.
"The American public is still unaware of the real value of acupuncture. Aside from treating chronic pain, such as back pain and neck pain, acupuncture has proved effective treating many other problems, such as stroke, arthritis and depression," she said.
Acupuncture stimulates the body to release endorphins, which block pain pathways in the brain, said Hu, who holds a doctorate from the Shanghai University of Traditional Chinese Medicine. While in China, she conducted research on more than 1,000 addiction patients and found acupuncture treatment effective, she said.
"However, there's a long way ahead for acupuncture to get into the mainstream," Hu conceded.
Acupuncturists in the US prefer to be paid in cash, partly because of insurance system complexities and partly because of low reimbursement rates, she said. Charges for acupuncture services can range from $65 to $150 per session, with a session usually lasting 45 minutes to an hour.
Hu's group recently organized a workshop to familiarize acupuncturists with the insurance system. Some 180 acupuncturists in the Bay Area attended.
Chunyan Su, who runs a clinic in Oakland, drove 64 kilometers to attend the workshop in Sunnyvale. "Most of my clients are car accident patients suffering from pain and numbness," she said. "They told us that accepting insurance can double our clients and revenues."
Another big challenge for acupuncturists is "dry needling", said Hu. Dry needling is a technique in which physical therapists use needles to treat pain and impairment of movement due to knotted muscles.
While acupuncture licensing in California requires 3,000 hours of classroom and clinical training, a physical therapist can practice dry needling after completing dozens of hours of training, according to Huang.
"Dry needling not only hurt the interests of acupuncturists but also poses health risks for patients," said Huang, vice-chairman of American Alliance for Professional Acupuncture Safety, a multistate union of acupuncture associations and schools.


