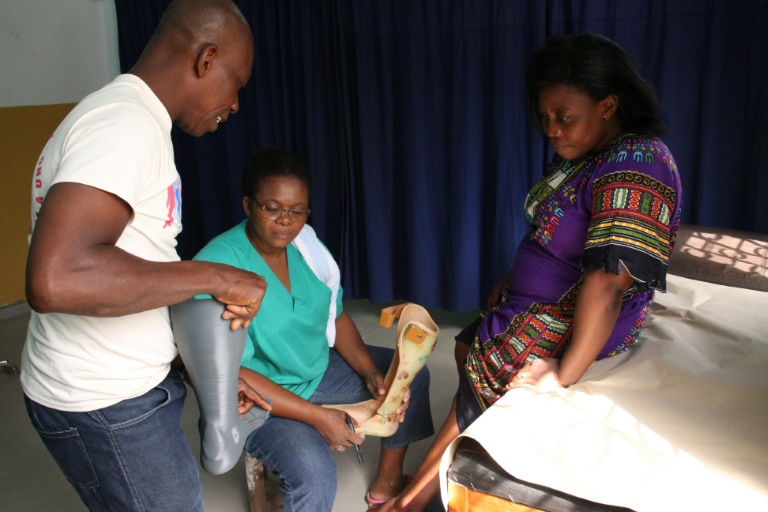
Car accident victim Adjovi Koudahe, 46, says she has 'high hopes' for her 3D-printed orthotic leg brace, here being fitted at Togo's national orthopaedic and physiotherapy centre.(Photo: AFP)
In a consulting room in Togo's capital, Lome, Geraldo Emmanuel -- handicapped since birth six years ago -- waits patiently on a bed while a digital scan is taken of his right leg.
Thanks to new 3D technology, he may be able to walk normally within a few months.
"The child walks on his toes so I'm scanning his leg so we can make him an orthotic using a 3D printer," said Enyonam Ekpoh, from Togo's national orthopaedic device and physiotherapy centre (CNAO).
A few hours later, Adjovi Koudahe, 46, has tests to receive a 3D brace for her right leg, which has been paralysed since a car accident in 2012.
"I've stopped doing anything because I'm in pain. I can't walk properly anymore," said the former trader, who limps heavily, aided by a crutch.
"Despite all the treatment I've had, my leg won't respond and drags along the ground. But with the brace they want to make here, I've got high hopes."
Three-dimensional printing is a fast-track way to make individually-tailored prosthetics and orthopaedic supports that compensate for a lack of a limb, deformity or paralysis.
The technology, initiated by a charity called Handicap International, allows the bespoke devices to be produced faster and reach a larger number of patients.
But if it is familiar to orthopaedic clinics in rich countries, it has yet to be introduced to poorer countries where needs are greater and the social safety net much smaller.
Only five to 15 percent of people in low income countries who need a prosthetic limb or orthopaedic brace get one, according to the non-profit organisation based in France.
Handicap International -- recently renamed Humanity & Inclusion -- is pushing ahead with research and clinical trials to see how the technology can be used in poor settings.
In 2016, it carried out clinical trials of three types of lower limb prosthetics in Madagascar, Syria and Togo, the results of which were highly encouraging.
A more ambitious project called "3D Impact" has been running in Togo, Mali and Niger since November last year, where 100 patients are getting made-to-measure 3D devices for free.
The project is backed by 700,000 euros ($816,000) of funding from the Belgian Development Agency.
Fifty of the 100 patients will be in Togo, where many handicaps affecting mobility are linked to strokes or infectious diseases such as polio, said Impact 3D manager Simon Miriel.
Saving time
3D printing is revolutionary for doctors working in conflict zones or even just hard-to-reach areas: the scanner is the size of about two mobile phones and very easy to transport.
One has been tested at a regional orthopaedic centre in Dapaong, some 620 kilometres (390 miles) by road north of the capital.
Normally, patients far from hospitals would have had to travel to have casts taken.
"It saves us a lot of time," said Miriel.
"As need be, scans can be sent directly by telephone to the specialist in charge of making the digital orthotic on a 3D printer."
In all, four 3D scanners are being used in the three countries.
Technician Fabrice Agbelehounko Djodji checks the work of a 3D printer used to produce prosthetic supports at the African Organisation for the Development of Centres for Disabled People in Lome. Making 3D devices locally is expected to cut costs.
The project's two printers are located in a laboratory in Avepozo, some 15 km from Lome, and work non-stop to produce all the orthopaedic devices.
Togo is a good choice, said Miriel. "It is one of the few countries in West Africa which has a good structure for orthopaedic care."
Specialists from across the region are trained at the national school of medical auxiliaries (ENAM), which is a partner in the project.
The test phase is expected to finish before the end of the year, and will be followed by a long evaluation about the successes and problems, costs and benefits.
But, if all goes well, the cost of 3D orthopaedic devices will fall dramatically, the charity hopes.
The devices that were tested in 2016 were printed overseas and cost between 1,500 and 2,000 euros each (from $1,745 to $2,330) -- a huge sum in West Africa, where the average wage often does not exceed $100 a month.
But once the devices are made in-country, they will become "a lot more accessible", said Miriel.


