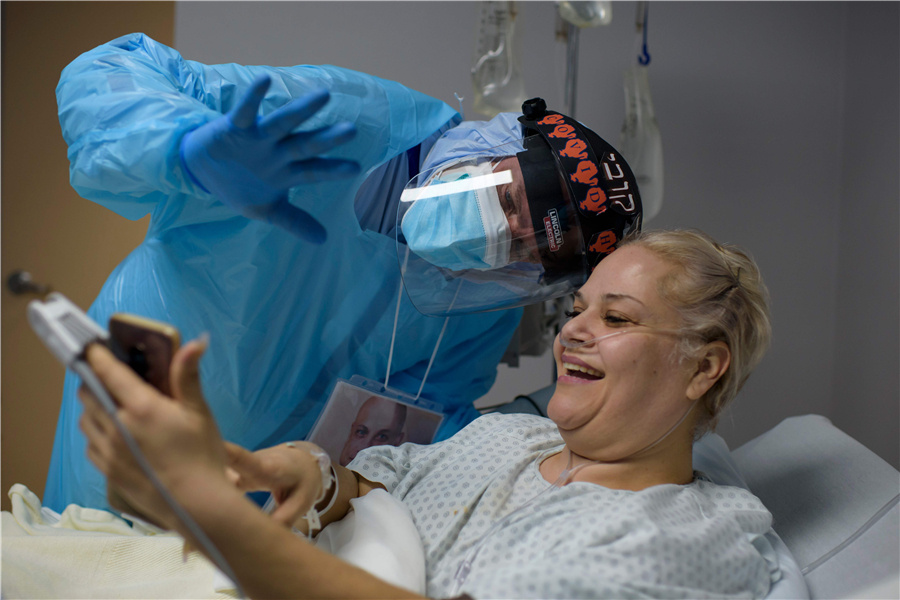
A COVID-19 patient receives treatment at a hospital in Houston, Texas. (Photo provided to CHINA DAILY)
Elmhurst Hospital in Queens, New York City, made headlines nationwide with stories of numerous deaths and photographs of bodies being placed in refrigerated trucks.
In March and April, "everyone was watching in horror what was happening in New York City and New Orleans, but that never seemed to arrive in rural America", said Brock Slabach, senior vice-president of the National Rural Health Association, according to the Fierce Healthcare website. "Over the summer, we thought perhaps rural areas were exempt from the impact of COVID-19."
With some exceptions, they were. In summer, the disease spread to suburban communities and ravaged the Sun Belt, which stretches across the south of the country from Florida to California. Rural areas again appeared to be free from the disease.
This is no longer the case.
The pandemic raging across the country is overwhelming hospitals of all sizes. The already-frayed healthcare safety net in rural areas is under attack from a "fall wave" of COVID-19 cases that has gone from bad to worse.
Nationwide, healthcare experts expect the latest wave to last until at least next month, surpassing the two previous ones in terms of the number of cases, hospitalizations and deaths.
Of the first 100,000 COVID-19 deaths in the US, about one-fifth occurred outside of urban areas. Nearly half of the second 100,000 deaths were among non-urban residents, according to an analysis by National Public Radio.
Slabach said the nation is now seeing higher mortality numbers in rural areas as the proportion of deaths in mid-size cities and rural communities rises.
Rural populations are often older, sicker and poorer than those in urban areas and have reduced access to physical and mental healthcare. This likely means that more rural residents infected with COVID-19 during this wave of cases will end up in hospitals.

To avoid physical contact, Santa Claus greets a child from inside an ice bubble in Oklahoma City, United States, on Dec 5, 2020. (Photo:Agencies)
COVID catching up to small facilities once largely unscathed
In Childress, Texas, people with COVID-19 symptoms seeking treatment at the local hospital are asked to wait in their cars when possible.
"They're either stacking up in the waiting room or out in the parking lot," said Holly Holcomb, chief operating officer for the Childress Regional Medical Center, adding that her six-bed emergency room has been stretched to the limit.
A man who arrived at the emergency room in October did not have COVID-19. However, his serious abdominal condition required surgery, hospital administrators told The Texas Tribune.
He waited more than nine hours in the emergency room while doctors called eight larger hospitals to see if they could perform the surgery, Holcomb said. They declined to accept the patient and the man died, the Tribune reported.
"I've been here 24 years and I don't ever remember not being able to transfer a patient out," said Holcomb, whose hospital in the town of about 6,900 is near the Oklahoma border.
The COVID-19 pandemic raging across the United States is overwhelming many hospitals, large and small, but especially the latter.
When the first wave of cases hit the country in March, rural communities were left largely unscathed.
The "beast", as New York Governor Andrew Cuomo called it, had made his state its epicenter.


